The female reproductive system is intricately designed for producing eggs, enabling fertility, supporting conception, facilitating pregnancy, and ultimately, childbirth․
Understanding its functions, historical research gaps, and hormonal influences is crucial for comprehensive reproductive health awareness and effective medical practices․
Historically, limited research focused on female anatomy, impacting knowledge; now, robust studies inform public health, policy, and sexual health initiatives․
Overview of Functions
The primary function of the female reproductive system revolves around the production of ova, or egg cells – essential components for potential fertilization and subsequent development of offspring․ Beyond this core role, the system is meticulously structured to facilitate conception, providing the environment where sperm and egg can unite․
Following fertilization, the uterus nurtures the developing fetus throughout pregnancy, offering protection and sustenance․ This system also prepares the body for childbirth, coordinating hormonal changes and physical adaptations necessary for labor and delivery․
Furthermore, the female reproductive system is intrinsically linked to hormonal regulation, producing estrogen and progesterone, which govern the menstrual cycle and influence various bodily functions․ Effective public health relies on understanding these functions․
Historical Context of Research
For decades, research concerning the female reproductive system lagged significantly behind studies focused on male anatomy․ Women were frequently excluded from medical research, leading to a substantial dearth of knowledge regarding female reproductive health and physiology․ This historical exclusion created a significant gap in understanding, hindering advancements in diagnosis and treatment․
Consequently, many aspects of female reproductive health remained poorly understood, impacting the development of effective public health programs and policies; The “feminine mystique” extended to a lack of scientific inquiry, perpetuating misconceptions and limiting healthcare options․
Recent efforts have aimed to rectify this imbalance, prioritizing inclusive research to address these historical shortcomings and improve women’s health outcomes․
External Female Reproductive Organs (Vulva)
The vulva encompasses the labia majora, labia minora, clitoris, and Bartholin’s glands, collectively serving protective and crucial roles in sexual function․
Labia Majora
The labia majora, meaning “larger lips,” are the outermost folds of skin that form the visible portion of the vulva․ These structures are homologous to the male scrotum, developing from the same embryonic tissue․
They extend downwards and backwards from the mons pubis, providing protection for the more delicate internal genital organs․ Composed of skin, subcutaneous fat, and glandular tissue, the labia majora are covered in pubic hair after the onset of puberty․
Their primary function is to shield the labia minora, clitoris, and vaginal and urethral openings from injury and infection․ They also contribute to sexual arousal and sensation, containing numerous nerve endings․ The size and appearance of the labia majora can vary significantly among individuals․
Labia Minora
The labia minora, or “smaller lips,” are two inner folds of skin located directly inside the labia majora․ Unlike their larger counterparts, they lack pubic hair and are generally more sensitive due to a higher concentration of nerve endings․
These delicate structures are highly vascularized, contributing to sexual arousal and lubrication․ They surround the clitoris and the openings of the urethra and vagina, providing protection and contributing to their sensitivity․
The labia minora are composed of specialized skin containing sebaceous and sweat glands․ Their size, shape, and color can vary considerably between individuals, and are influenced by genetics and hormonal factors․ They play a crucial role in sexual function and overall vulvar health․
Clitoris
The clitoris is a small, sensitive organ located at the upper junction of the labia minora, and is primarily dedicated to sexual pleasure․ It’s the most concentrated area of nerve endings in the human body, making it highly responsive to stimulation․
Externally, the visible portion is called the glans, covered by a retractable hood called the prepuce․ Internally, the clitoris extends into structures analogous to the male penis, including the corpora cavernosa and bulb․
During sexual arousal, blood flow increases to the clitoris, causing it to become engorged and sensitive․ It plays a central role in female sexual response and orgasm․ Its function is solely for sexual pleasure, unlike other reproductive organs․
Bartholin’s Glands
Bartholin’s glands are two pea-sized glands located on either side of the vaginal opening, nestled within the labia minora․ Their primary function is to secrete a small amount of fluid that helps lubricate the vagina during sexual arousal;
This fluid, a clear, mucus-like substance, contributes to vaginal moisture, facilitating comfortable and pleasurable sexual intercourse․ The ducts of these glands open just outside the hymen․
Occasionally, the ducts can become blocked, leading to a Bartholin’s cyst․ If the cyst becomes infected, it can develop into an abscess, causing pain and discomfort․ Treatment typically involves drainage or, in recurrent cases, surgical removal․

Internal Female Reproductive Organs
Internal organs – ovaries, fallopian tubes, uterus, and vagina – are vital for oocyte production, fertilization, gestation, and childbirth, working in harmony․
Ovaries
Ovaries are essential gonads, responsible for producing and releasing ova (eggs) and synthesizing crucial reproductive hormones like estrogen and progesterone․
These almond-shaped organs are located on either side of the uterus and are intrinsically linked to the female reproductive cycle and fertility․
Within the ovaries reside ovarian follicles, sac-like structures that nurture developing oocytes․ This process, oogenesis, involves the maturation of these cells․
Follicles progress through stages, culminating in ovulation – the release of a mature egg․ Hormone fluctuations regulate follicular development and ovulation․
After ovulation, the remnants of the follicle transform into the corpus luteum, which produces progesterone to prepare the uterine lining for potential implantation․
Understanding ovarian function is paramount for comprehending female reproductive health, fertility, and hormonal balance throughout a woman’s life․
Ovarian Follicles and Oogenesis
Ovarian follicles are fluid-filled sacs within the ovaries that house and nurture developing oocytes, or egg cells․ These follicles represent different stages of maturation․
Oogenesis, the process of egg cell formation, begins before birth with primordial germ cells undergoing meiosis․ This complex process ensures genetic diversity․
Primordial follicles mature into primary, secondary, and finally, Graafian follicles, each stage marked by changes in size and structure․
Only one follicle typically reaches full maturity each menstrual cycle, releasing a mature oocyte during ovulation․
Meiosis is arrested at several points during oogenesis, resuming only with hormonal stimulation․ This regulated process is vital for proper egg development․
The remaining follicular cells contribute to hormone production, particularly estrogen, crucial for regulating the menstrual cycle and preparing for potential pregnancy․
Fallopian Tubes
Fallopian tubes, also known as uterine tubes, extend from the ovaries to the uterus, serving as the pathway for the oocyte and the site of fertilization․
These muscular tubes are approximately 10-13 cm long and are not directly attached to the ovaries, allowing for oocyte capture․
The fimbriae, finger-like projections at the ovarian end, sweep over the ovary’s surface, guiding the released oocyte into the tube․
The ampulla, the widest section of the tube, is the typical location for fertilization by sperm․
Cilia lining the fallopian tubes and peristaltic contractions propel the oocyte towards the uterus․
The isthmus, the narrowest portion, connects to the uterus, facilitating oocyte or early embryo transport․
Fimbriae
Fimbriae are finger-like projections located at the distal end of the fallopian tubes, closest to the ovaries, playing a crucial role in oocyte capture;
These delicate, ciliated structures sweep the ovarian surface, creating currents that draw the released oocyte into the fallopian tube after ovulation․
The fimbriae aren’t directly attached to the ovary, allowing for movement and effective capture, even with slight ovarian positioning changes․
Cilia, tiny hair-like structures, beat rhythmically, generating the fluid currents essential for oocyte transport․
The fimbriae’s coordinated movements increase the probability of successful oocyte retrieval, vital for potential fertilization․
Their structure and function are essential components of female reproductive capability, ensuring the egg reaches the ampulla․
Ampulla
The ampulla represents the widest section of the fallopian tube, serving as the primary site for fertilization within the female reproductive system․
Its spacious lumen provides ample room for the sperm to ascend and encounter the oocyte, released from the ovary and transported by fimbriae․
The ampulla’s inner lining is composed of ciliated cells and secretory cells, facilitating oocyte movement and providing a nurturing environment․
Fertilization typically occurs within the ampulla’s confines, initiating the development of a zygote, the first stage of embryonic life․
Peristaltic contractions of the fallopian tube’s muscular wall further aid in transporting the fertilized egg towards the uterus․
The ampulla’s structure is optimized for successful fertilization, a critical step in human reproduction․
Uterus
The uterus, often called the womb, is a pear-shaped muscular organ centrally located within the female pelvis, playing a vital role in menstruation, pregnancy, and childbirth․
Its primary function is to nurture a developing fetus, providing a protective and nourishing environment throughout gestation․
The uterus is connected to the fallopian tubes superiorly and the vagina inferiorly, forming a continuous pathway for reproductive processes․
Its muscular walls, capable of significant expansion, accommodate the growing fetus during pregnancy and facilitate labor contractions․
The uterine lining undergoes cyclical changes during the menstrual cycle, preparing for potential implantation of a fertilized egg․
This dynamic organ is essential for female reproductive capability and overall health․
Uterine Layers (Endometrium, Myometrium, Perimetrium)
The uterine wall comprises three distinct layers: the endometrium, myometrium, and perimetrium, each with specialized functions crucial for reproductive processes․
The endometrium, the innermost layer, undergoes cyclical changes in response to hormones, preparing for implantation; it’s shed during menstruation․
The myometrium, the muscular middle layer, is responsible for uterine contractions during labor and delivery, exhibiting significant strength and elasticity․
The perimetrium, the outer serous layer, provides a protective covering for the uterus, connecting it to surrounding pelvic structures․
These layers work in coordinated harmony to support fetal development and ensure successful reproductive outcomes․
Understanding these layers is fundamental to comprehending uterine physiology and pathology․
Vagina
The vagina is a fibromuscular canal extending from the uterus to the external genitalia, serving multiple reproductive functions․
It acts as the passageway for menstrual flow, receives the penis during intercourse, and forms the birth canal during childbirth․
The vaginal walls possess remarkable elasticity, allowing for expansion during sexual activity and delivery․
Its lining contains numerous rugae, or folds, which contribute to its distensibility and provide a large surface area․
The vagina maintains a slightly acidic pH, protecting against harmful bacteria and infections․
Lubrication, facilitated by Bartholin’s glands, ensures comfortable intercourse and eases childbirth․

The Menstrual Cycle
The menstrual cycle is a recurring monthly process preparing the female body for potential pregnancy, involving hormonal fluctuations and uterine changes․
It’s characterized by distinct phases – menstrual, follicular, ovulatory, and luteal – each governed by specific hormonal signals․

Phases of the Menstrual Cycle
The menstrual cycle unfolds in four key phases, each with distinct physiological events․ The menstrual phase marks the shedding of the uterine lining, resulting in bleeding, typically lasting 3-7 days;
Following this, the follicular phase begins, where follicles in the ovaries mature, stimulated by Follicle-Stimulating Hormone (FSH), and the uterine lining thickens․
The ovulatory phase sees the release of a mature egg from the ovary, triggered by a surge in Luteinizing Hormone (LH), making conception possible․
Finally, the luteal phase involves the corpus luteum forming after ovulation, producing progesterone to further prepare the uterine lining for implantation; if fertilization doesn’t occur, the cycle restarts․
Menstrual Phase
The menstrual phase, typically lasting 3 to 7 days, signifies the beginning of the menstrual cycle․ During this phase, the uterine lining, known as the endometrium, is shed through the vagina, resulting in menstrual bleeding․
This shedding occurs because of declining levels of estrogen and progesterone from the previous cycle, signaling the body that pregnancy has not occurred․
Alongside the shedding, the uterus contracts to help expel the lining․ Common symptoms experienced during this phase include cramps, bloating, and mood swings, varying in intensity among individuals․
It’s a natural and essential process, marking the preparation for a potential new cycle of ovulation and possible fertilization․
Follicular Phase
The follicular phase, spanning approximately 13-14 days, begins with the first day of menstruation and prepares the body for ovulation․ During this phase, the pituitary gland releases follicle-stimulating hormone (FSH), stimulating the growth of ovarian follicles․
Each follicle contains an immature egg, and typically, one dominant follicle emerges, maturing and preparing to release an egg․
As the follicles develop, they produce increasing amounts of estrogen, which causes the uterine lining (endometrium) to thicken in preparation for potential implantation․
Rising estrogen levels also provide feedback to the pituitary gland, eventually triggering a surge in luteinizing hormone (LH), initiating the next phase․
Ovulatory Phase
The ovulatory phase is a brief, yet critical, period typically lasting 16-24 hours․ Triggered by a surge in luteinizing hormone (LH), the dominant follicle ruptures, releasing a mature egg – the ovum – from the ovary․
This release marks the peak of fertility, as the egg travels into the fallopian tube, awaiting potential fertilization by sperm․
Basal body temperature often slightly increases during ovulation, and cervical mucus becomes clearer and more elastic, facilitating sperm transport․
The surge in LH is a direct response to rising estrogen levels during the follicular phase, creating a positive feedback loop essential for egg release and reproductive success․
Luteal Phase
The luteal phase commences immediately after ovulation, lasting approximately 14 days; Following the egg’s release, the ruptured follicle transforms into the corpus luteum, a temporary endocrine structure․
The corpus luteum primarily produces progesterone, alongside some estrogen, preparing the uterine lining (endometrium) for potential implantation of a fertilized egg․
Progesterone thickens the endometrium, making it receptive to a developing embryo, and also inhibits further ovulation․
If fertilization doesn’t occur, the corpus luteum degenerates, causing progesterone and estrogen levels to decline, ultimately triggering menstruation and the start of a new cycle․
Hormonal Control of the Menstrual Cycle
The menstrual cycle is meticulously orchestrated by a complex interplay of hormones, primarily estrogen, progesterone, follicle-stimulating hormone (FSH), and luteinizing hormone (LH)․
FSH, released from the pituitary gland, stimulates ovarian follicle development, each containing an egg․ As follicles grow, they produce estrogen, thickening the uterine lining․
Rising estrogen levels trigger an LH surge, prompting ovulation – the release of a mature egg․
Post-ovulation, the corpus luteum produces progesterone, maintaining the uterine lining․ Declining hormone levels, if fertilization doesn’t occur, initiate menstruation, restarting the cycle․
Estrogen
Estrogen is a pivotal hormone, primarily produced by the developing ovarian follicles, profoundly influencing the female reproductive system and beyond․ It’s responsible for the development of female secondary sexual characteristics during puberty, including breast growth and widening of the hips․
Crucially, estrogen stimulates the thickening of the uterine lining (endometrium) during the follicular phase of the menstrual cycle, preparing it for potential implantation․
Rising estrogen levels also provide feedback to the pituitary gland, regulating FSH and LH secretion․
Beyond reproduction, estrogen impacts bone health, cardiovascular function, and even cognitive processes, demonstrating its widespread systemic effects․
Progesterone
Progesterone, predominantly secreted by the corpus luteum after ovulation, plays a vital role in preparing and maintaining the uterus for pregnancy․ It transforms the thickened endometrium into a secretory lining, crucial for successful implantation of a fertilized egg․
During the luteal phase, progesterone levels rise, suppressing further ovulation and preventing new follicular development․
If fertilization doesn’t occur, the corpus luteum degrades, progesterone levels decline, triggering menstruation․
Progesterone also contributes to the development of mammary glands during pregnancy, preparing for lactation․ Its influence extends beyond reproduction, impacting mood and body temperature regulation․
Follicle-Stimulating Hormone (FSH)
Follicle-Stimulating Hormone (FSH), released by the pituitary gland, initiates follicular growth in the ovaries during the follicular phase of the menstrual cycle․ It stimulates the development of ovarian follicles, each containing an immature egg, or oocyte․
FSH levels gradually rise in the early follicular phase, prompting several follicles to begin maturation, though typically only one becomes dominant․
As follicles grow, they produce estrogen, creating a negative feedback loop that eventually suppresses FSH secretion․
FSH is essential for proper ovarian function and fertility, and its levels are often monitored in fertility treatments to optimize egg development․
Luteinizing Hormone (LH)
Luteinizing Hormone (LH), also secreted by the pituitary gland, plays a pivotal role in triggering ovulation and the development of the corpus luteum․ A surge in LH levels, occurring mid-cycle, prompts the dominant follicle to release its mature egg – ovulation․
Following ovulation, LH stimulates the remaining follicular cells to transform into the corpus luteum, which produces progesterone․
Progesterone prepares the uterine lining for potential implantation of a fertilized egg․
LH levels decline if fertilization doesn’t occur, leading to the corpus luteum’s degeneration and the onset of menstruation․ Monitoring LH surges is crucial for timing intercourse or assisted reproductive technologies․
Fertilization and Pregnancy
Fertilization begins with sperm interacting with the ovum, potentially leading to implantation and the initiation of pregnancy—a complex, transformative process․
Ovum and Sperm Interaction
The journey begins with capacitation, where sperm undergo changes enabling fertilization within the female reproductive tract․ Millions embark, but only a few reach the ampulla of the fallopian tube, where the ovum awaits․
Sperm penetration involves navigating the corona radiata and zona pellucida surrounding the egg, aided by enzymes released from the acrosome․ Once a sperm successfully penetrates, the ovum undergoes cortical reactions, preventing polyspermy—fertilization by multiple sperm․
Genetic material merges as the sperm’s nucleus enters the ovum, forming a zygote with a complete set of chromosomes․ This single cell marks the beginning of a new individual, initiating the cascade of events leading to embryonic development and, ultimately, pregnancy․
Implantation
Following fertilization, the zygote undergoes rapid cell division, transforming into a morula and then a blastocyst—a hollow ball of cells․ Approximately six to twelve days post-fertilization, the blastocyst reaches the uterus, seeking a suitable location for implantation․
The endometrium, the uterine lining, prepares for implantation under hormonal influence, becoming richly vascularized and receptive․ The blastocyst adheres to the endometrium, and its outer cells, the trophoblast, invade the uterine tissue․
Successful implantation establishes a connection between the developing embryo and the maternal blood supply, crucial for nutrient and oxygen exchange․ This process triggers hormonal changes supporting the continuation of pregnancy, marking a pivotal moment in early development․

Reproductive Health and Common Conditions
Maintaining reproductive health involves preventing STIs, managing conditions like PCOS, and ensuring regular check-ups for early detection and effective treatment options․
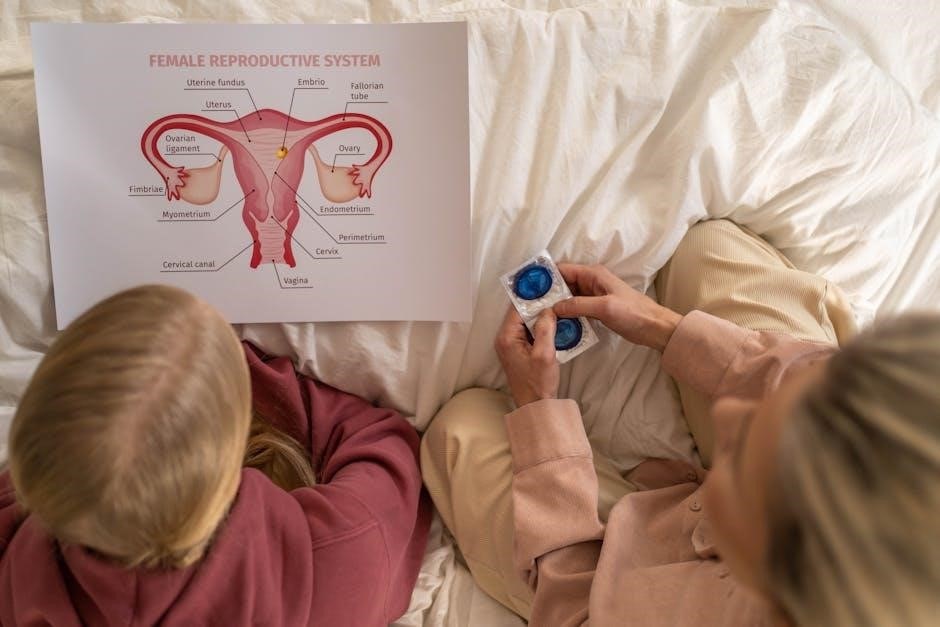
Sexually Transmitted Infections (STIs)
Sexually transmitted infections (STIs) pose a significant threat to female reproductive health, often presenting unique challenges due to the anatomy of the system․
Untreated STIs, such as chlamydia and gonorrhea, can lead to Pelvic Inflammatory Disease (PID), causing chronic pain, infertility, and ectopic pregnancy risks․
Regular screening is vital, even in the absence of symptoms, as many infections initially display no noticeable signs․ Early detection allows for prompt treatment, preventing long-term complications․
Effective public health programs, research, and policies are essential for STI prevention, education, and access to care, impacting overall reproductive well-being․
HIV transmission also requires focused prevention strategies, including safe sex practices and pre-exposure prophylaxis (PrEP) where appropriate․
Polycystic Ovary Syndrome (PCOS)
Polycystic Ovary Syndrome (PCOS) is a common hormonal disorder affecting women of reproductive age, characterized by irregular periods, excess androgen levels, and/or polycystic ovaries․
This condition can disrupt ovulation, leading to infertility and challenges in achieving pregnancy․ Symptoms vary widely, including hirsutism (excess hair growth), acne, and weight gain․
PCOS is often associated with insulin resistance, increasing the risk of type 2 diabetes and cardiovascular disease․ Diagnosis typically involves a physical exam, hormone testing, and ultrasound․
Management focuses on symptom control through lifestyle modifications, medication to regulate periods, and treatments to address infertility concerns․

Early diagnosis and comprehensive care are crucial for managing PCOS and minimizing long-term health risks․

